Periodontology
Periodontology focuses on the prevention, diagnosis, and treatment of diseases affecting the supporting structures of the teeth. These include the gingiva, periodontal ligament, cementum, and alveolar bone. The field mainly addresses conditions such as gingivitis and periodontitis. If left untreated, these conditions may lead to attachment loss and eventual tooth loss.
In addition, periodontology includes the maintenance of periodontal health and the management of risk factors. It also considers the relationship between periodontal and systemic conditions. Treatment ranges from non-surgical approaches, such as scaling and root surface debridement, to surgical procedures, including regenerative and resective techniques.
Overall, periodontology plays a key role in preserving natural dentition and supporting long-term oral and general health.

Implantology
Implantology focuses on the replacement of missing teeth using dental implants. These implants are biocompatible devices placed in the jawbone to support fixed or removable prostheses. The process involves careful patient assessment, detailed treatment planning, and precise surgical placement. This is followed by prosthetic restoration to restore both function and aesthetics.
Moreover, implantology includes the study of bone biology and osseointegration. It also requires careful management of hard and soft tissues to achieve stable outcomes. In addition, clinicians must prevent and manage complications such as peri-implant disease and implant failure.
Therefore, implantology plays a central role in modern restorative dentistry and offers predictable solutions for tooth loss.

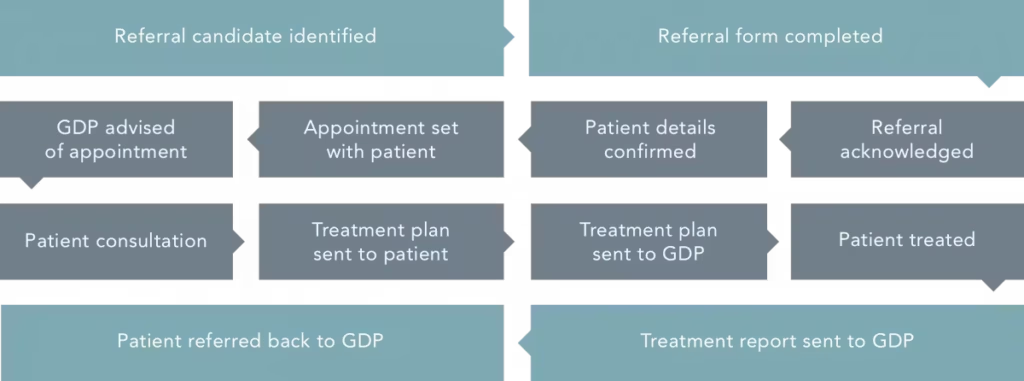
Diagnosis and Referral
Diagnosis and referral form a critical part of dental care. Clinicians assess clinical signs, symptoms, medical history, and radiographic findings to reach an accurate diagnosis. This process also helps determine the severity and complexity of disease.
When a case exceeds the scope of general practice, referral becomes necessary. In such cases, clinicians must clearly communicate their findings and justify the referral. They must also coordinate care effectively to support optimal outcomes.
Consequently, timely diagnosis and appropriate referral help prevent disease progression and reduce complications. They also ensure that patients receive the most appropriate level of care.
Treatment Planning
Treatment planning is a structured process that integrates clinical findings, patient history, and diagnostic data. It allows clinicians to develop an appropriate and individualised plan of care. At the same time, they must consider disease severity, risk factors, functional needs, and aesthetic expectations.
A comprehensive plan outlines treatment options, sequencing, and expected outcomes. Furthermore, it ensures that care remains evidence-based and aligned with accepted standards. Clinicians must also include informed consent, patient preferences, and long-term maintenance strategies.
Ultimately, effective treatment planning supports predictable outcomes while minimising risk. It also forms the foundation for safe clinical decision-making.

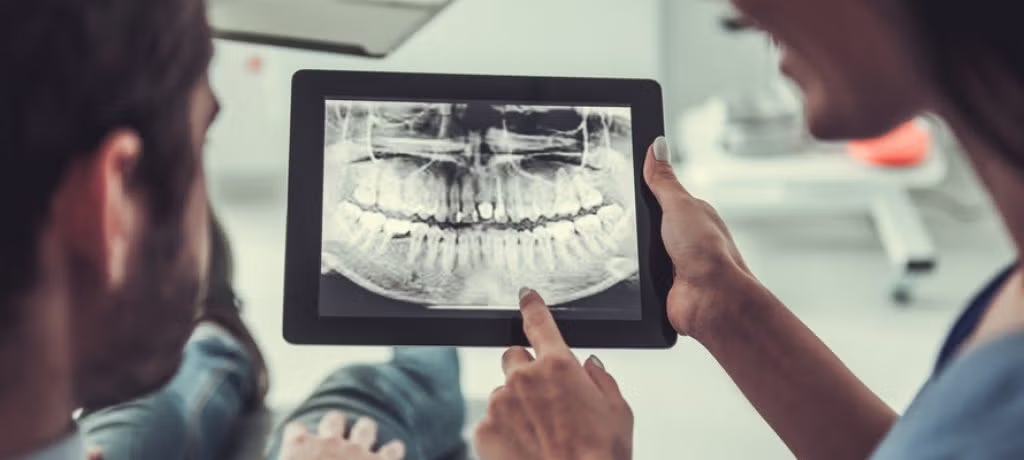
Radiographic Interpretation
Radiographic interpretation plays a key role in diagnosis and management. Clinicians analyse imaging such as periapical, bitewing, and panoramic radiographs. This allows them to assess bone levels, anatomical structures, and pathological changes.
In addition, radiographs help detect conditions that may not be clinically visible. These include periodontal bone loss, peri-implant changes, and other pathology. They also support treatment planning, risk assessment, and ongoing monitoring.
Therefore, accurate interpretation, combined with clinical findings, ensures informed decision-making and safe patient care.
Maintenance and Prognosis
Maintenance and prognosis are essential for long-term success. Ongoing supportive care includes regular monitoring, professional debridement, and reinforcement of oral hygiene. Clinicians also assess and manage risk factors such as smoking, systemic health, and patient compliance.
Prognosis depends on disease severity, response to treatment, and tissue stability over time. In addition, clinicians consider both local and systemic factors. They also evaluate the patient’s ability to maintain adequate plaque control.
As a result, a structured maintenance programme supports long-term stability and helps prevent recurrence.
